Nasal decolonization in ambulatory care: Evidence & strategies
Watch this webinar to review the evidence for nasal decolonization, highlight the success in preventing surgical site infections and explore the benefits of universal decolonization.
Transcript
Brandon Martin: Good afternoon, everyone, and welcome to the McKesson Medical-Surgical Webinar Wednesday presentation. My name is Brandon Martin. I'm the customer engagement manager at McKesson Medical-Surgical, and I'm pleased to welcome you to our event. Today's conference is being recorded. To ask a question over the web during today's program, please locate the Q&A panel in the lower left corner of your console. Once open, type in your question and click "send to all panelists".
Today's presentation is "Nasal decolonization in ambulatory care: Evidence and strategies", and our speaker today, Marc-Oliver Wright, comes to us from PDI Healthcare, Inc. Marc-Oliver Right is the clinical science liaison for the central region at PDI Inc. He has an extensive work history in infection prevention, including as an infection preventionist at the University of Wisconsin University Hospital in Madison, Wisconsin, and corporate director of Infection Control and Quality Improvement for Northshore University Health System in Evanston, Illinois. His educational background includes a Bachelor of Sciences in Clinical Laboratory Sciences, a Master of Science in epidemiology and advanced training in public health informatics. He is board certified in infection prevention and control, as well as certified as a medical technologist. He is a fellow of the Association for Professionals in Infection Control and Epidemiology, or APIC, served as an officer and member of the Board of Directors for APIC. He has authored several book chapters, including in APIC's Surveillance Programs for Healthcare Settings and SHEA's Practical Healthcare Epidemiology. He has over 60 publications in the American Journal of Infection Control and Hospital Epidemiology, Emerging Infectious Diseases, among others, and served as an editorial board member and section editor for the American Journal of Infection Control from 2009 to 2019.
Before we begin the presentation, a few quick notes. PDI has provided information on obtaining continuing education credits that we will share with you via email along with a PDF version of the presentation. If time allows, we will have a brief Q&A at the end of the presentation, but we do have a full hour of content. We thank you so much for your time today. And please join me in welcoming Marc-Oliver Wright.
Marc-Oliver Wright: Well, good afternoon, everyone, and thank you very much to McKesson for the opportunity to speak with you today. By way of disclosures, I am currently employed at PDI. Prior to joining the company nearly two years ago, I spent the preceding 20 years working in infection prevention. And while I'm employed by a commercial entity and this presentation will discuss general product categories, there's going to be no specific commensal entities or products named. While this presentation does have a focus on ambulatory care settings, and specifically ambulatory surgery centers approximately halfway through, I would be remiss if I didn't say at the outset the vast majority of science supporting the use of nasal decolonization comes to us from the acute care, and even to a limited extent, the long-term care setting. But as our care model shifts and changes, so too should our patient safety efforts, all with the same goal in mind: safe, effective, patient-centered care for population health.
So the average human adult human body is comprised of slightly more than 30 trillion cells. These make up your bones, organs, hair, eyes and skin - the cells that make you you. Delightfully housed on that skin and in some internal parts of our body is a multiverse of over 39 trillion bacterial and microbiologic cells. We're basically walking germplasms, outnumbered yet existing in a more or less symbiotic state with our microscopic passengers.
Suffice to say, our outnumbered state is a welcomed one in most circumstances. However, when this symbiotic relationship is disrupted, when we offer our microscopic passengers a more rich environment in which to grow and multiply, we incur that wrath of infection. Our body's natural defenses - such as the intact skin or the cilia lining our respiratory tract - when these defenses are circumvented through incision, intubation or catheterization, we're effectively putting in a superhighway for these organisms to travel to more nutrient-rich environment. Of course, these disruptions are usually medically necessary - that's why we do them. Which actually brings us to the main topic of this presentation: strategies to effectively mitigate infection from the self-inoculation of our own microbiomes. So these are actually our objectives for this afternoon, and these were hopefully made available to you in advance.
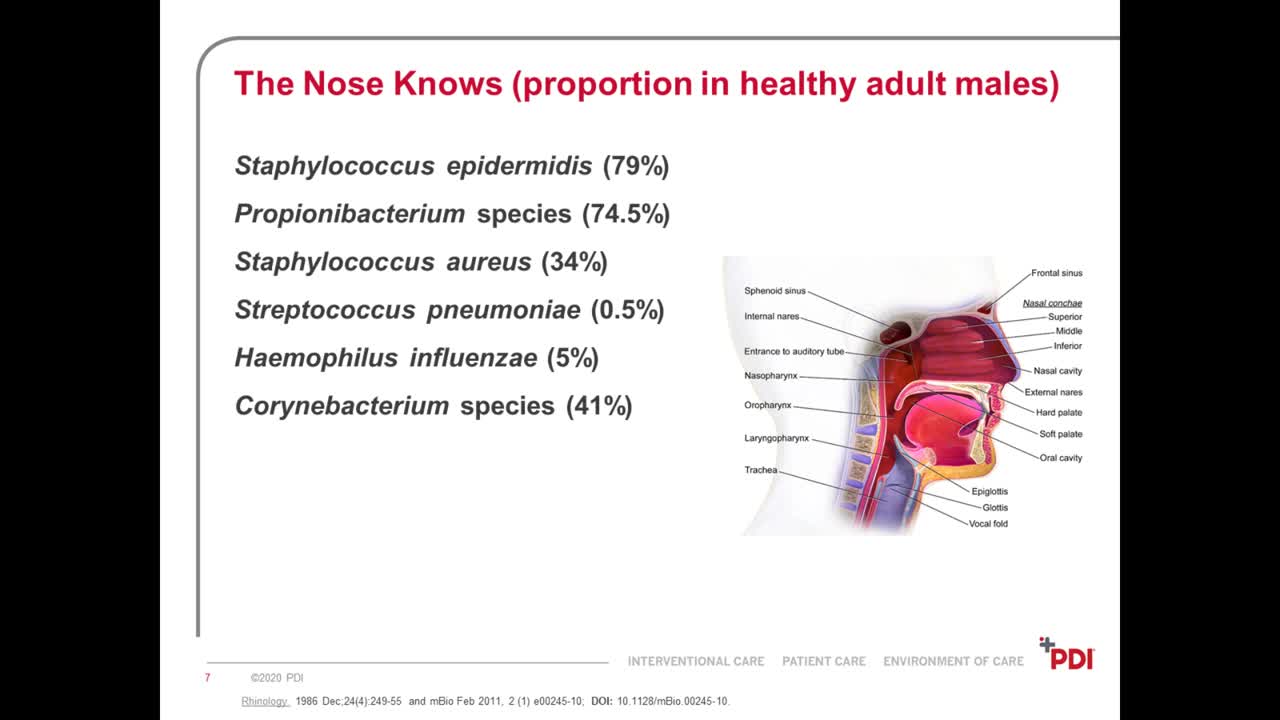
Now here we see the distribution and phylogenetic variation of bacterial organisms in that single anatomical site of the human nares[?], clearly predominated by gram-positive organisms. This relatively normal, relatively healthy flora is usually established within the first year of birth, but can vary throughout our lifetime. For example, with children three years of age and younger, the most common isolated group of organisms isn't even on this list. It's called moraxellaceae[?]. And actually the second most common in this young group is streptococcus species, which, as you can see here, is least dominant in adults. Yet staph and strep aren't the only organisms.
While the distribution of species can vary among individuals and within the same individual over time, the nares is nearly never vacant. The composition and variation of the flora in our nose is thought to be influenced by host-specific factors as well as environmental factors. There's actually some really interesting stuff with this. There's theoretically a bacteria-to-bacteria interaction that goes on. For example, it is thought that persons who are colonized with streptococcus pneumoniae are less likely to be chronically colonized with staph aureus, because actually streptococcus strains produce a modest amount of hydrogen peroxide, which actually creates an antagonistic environment for staph. But does nares colonization actually cause or precede infection?
Well, in acute care coagulase-negative staphylococci species is the number one recovered organism in the nose and the number one cause of collapsing in the ICU and the number four cause of SSI. Of course, staph aureus is less prevalent in the nose, but still present in over a third of specimens, and it's actually the number one pathogen for surgical site infection in pneumonia. It's the number one pathogen for a central line associated bloodstream infections in non-critical-care settings and actually the number two overall for all HAIs. And some proportion of staph aureus is obviously going to be resistant - by that I mean MRSA or methicillin resistant staph aureus. And this seems to implicate a potential cause and effect. But is that true?
Well, colonization can and does precede infection, and often with a high degree of correlation. In three separate studies, correlation between nares colonization and staphylococcus aureus, and that ensuing staphylococcus aureus infection of the surgical site or bloodstream or the lungs were all in excess of 80%. And of course, these studies focused on staph aureus, and there is an abundance of information out there focusing on that subset of strains that are MRSA. But as we saw a moment ago, the nares is a poly-microbial environment.
Well, I wouldn't say that words[?] actually matter. This may seem unnecessarily basic, but the distinctions between these terms are critical for this presentation. A moment ago, we showed how the human nose is heavily colonized with a panacea of organisms, and how this develops early in life and how it changes and evolves in our lifetime. The nares is not a sterile space. This is inherently normal. And while it increases the risk of infection when we disrupt the equilibrium through medical interventions, colonization in itself is not[?] a disease state. Therefore, it does not[?] necessarily warrant a cure.
Not listed here is disinfection which sometimes gets conflated with decolonization. You can't actually disinfect any part of the living human body. So we definitely don't want to use that term. And just as importantly, while it may be possible to rid the anatomical site of one or more particular organisms, this is often transient or come with potential unintended consequences to that human microbiome overall. Decolonization is fundamentally about decreasing the bacterial burden, often at particular time periods of high risk, such as pre-surgically, in order to prevent transmission to others and or infection to the self or others. When we talk about persistence of different strategies later on, I'm going to come back to this topic. For the purposes of this presentation, decolonization will - unless I say otherwise - refer to both nares decolonization as well as bathing the skin of the patient with a chlorhexidine-based solution.
So while Dr. Perl and colleagues at Johns Hopkins University first reported the effectiveness of SSI reduction with nares colonization alone - in other words, without bathing protocols and they used mupirocin way back in 2002. This study that came out eight years later incorporated CHG bathing in addition to the nares treatment. Importantly, in this double-blinded, randomized controlled clinical trial, they screened all admissions to the hospital for staph aureus. They randomized positive patients to CHG mupirocin or a placebo effect, and then look for any or all infections caused by staph aureus, and they saw a 58% reduction in the treated group as opposed to the placebo non-decolonized group. I'd call your attention to the 18% colonization rate - it's pretty low. But also worth noting the reason there was a focus on susceptible staph aureus because there was hardly any MRSA in Netherlands due to a very aggressive national strategy.
Well, what about bloodstream infections? Well, there have been a lot of studies done, and here I highlight four of my favorites. Back in 2003, there was a meta analysis that showed a 78% reduction in staph aureus bacteremia among dialysis patients. And then ten years later, the reduced MRSA trial showed a 44% reduction of any and all organisms caused by bloodstream infection. Again, the nares, like the skin, is polymicrobial after all. And this was actually repeated three years later in 95 community hospitals with similar results. And then the largest trial to date of 523 facilities and 339,000 patients, decolonization showed a reduction reported to be 32%.
So aforementioned[?] slide[?] contributed in part to these core strategies from the Centers for Disease Control and Prevention to prevent staphylococcus bloodstream infections in acute care. And as you can see, they recommend universal ICU decolonization as a strategy for ICU patients during high-risk periods, and they recommend a supplemental strategy for patients with invasive catheters outside of the ICU. They recommend two strategies for nasal decolonization in conjunction with daily CHG bathing. We'll get into the methods in just a second.
So we've saved the most commonly studied HAI for last - the surgical patient population. Well, first of all, surgical site infections, or SSIs, are among the most multifactorial healthcare complications that can possibly occur. Broadly speaking, risk factors can be at the organization or facility level and at the host or patient-specific level. Even within these broad categories, there are a multitude of specific subsets. For example, opportunities for infection occur in the pre-op setting, including pre-outpatient instructions, how they adhere to them, bathing or skin prep, how we remove the hair or if we remove the hair, or utilization and selection of antimicrobial prophylaxis. Intra-operatively, there are considerations such as surgical approach, technique or traffic, engineering controls within the operating suite, as well as, of course, hand hygiene and adherence to best practice as well as closure techniques. And then post-operative opportunities for infection exist the facility level as well, from surgical dressing technique and manipulation and hand hygiene, as well as post-discharge care again, with patient instructions and how well they adhere to them. There are also, though, host-specific factors that can include multiple comorbidities, which can increase that risk of infection, like body mass index, diabetes, smoking. The potential infectious causes are a wide array of modifiable and less modifiable risks, and as such, we have to focus on the conditions we can control to optimize the patient's opportunity to recover without infection.
This systemic review and meta analysis published back in 2013 from Schweizer and colleagues at the University of Iowa sums up the evidence supporting nares decolonization pre-operatively quite nicely. These were 17 studies, which included seven studies that decolonize only the nose, mostly with mupirocin and focused on gram-positive organisms exclusively with only orthopedic and cardiac surgery procedures. There was a significant protective effect with nares decolonization, regardless of whether or not that decolonization targeted known staph aureus carriers or not. While you can see that at the individual study level, some studies overlap, one, lacking statistical significance, the majority of studies and all the studies collectively overall found a protective effect, and this effect was statistically significant.
Well, what about other procedures beyond cardiac and orthopedics? Here are two reports of SSI reductions in neurosurgery, as one report - along with one report of colorectal surgeries at Virginia Commonwealth University. And they all tend towards the same direction: that decolonization reduces the risk of surgical site infection. Added to that, Dr. Richard Wenzel, in a recent literature review, has concluded upwards of 70% to 95% of all SSIs originate from the microbiome of the patient's own skin or nares, further reinforcing the critical role of appropriate surgical skin antisepsis, but decolonization as well.
Well, while no one disputes the fact that staph aureus species, including - or staph species, including staph aureus, causes the majority of SSIs, in this review including NHS data of adult procedures between 2009 and 2014, they accounted for approximately 30% of the causing organisms. As we noted from Dr. Wenzel's review, more than 70% of SSIs originate from the patient's own flora.
The preponderance of evidence supporting decolonization for the prevention of surgical site infection comes to us from cardiac, orthopedic, and to a lesser extent, neurosurgical and colectomy procedures. The vast majority of studies looking at this question have focused on using mupirocin for nares decolonization. The table shown here is from the 1985 publication that evaluated the effectiveness of mupirocin. Undoubtedly in the last 35 years, these numbers have not gotten any better. So this effectiveness of mupirocin represents what we would call the very best case scenario. And as you can see under this best case scenario, mupirocin is effective against staph and many strep species, but not group D strep, or what we actually now call enterococcus. It's not effective against corynebacterium or propionibacterium, as you saw in the nose slide earlier, and with the exception of haemophilus and neisseria, it's not really effective against the gram-negative organisms. So why does decolonization work for cardiac, ortho, neuro cases, and not so much for others? It's a good question, isn't it?
Well, here we see the percent of microorganisms by NHSN procedure type for 9,858 surgical site infections throughout Europe between 2014 and 2016 for CABGs, joint replacements and laminectomies, gram-positive organisms cause the vast majority of the infections. And among that large group, the staphylococcus species account for about 50% of those infections. Now, compare and contrast that in red where the corresponding predominant pathogens or gram-positive organisms impacted by mupirocin to the varying degrees, with cholecystectomies or colectomies or caesarean sections, where, despite the relative proximity of the incision, the organisms are more diverse - in green and orange. Of course, not all surgical site infections originate in the nose - that would be silly. But it may explain in part why decolonization studies focused on using limited spectrum antimicrobials are demonstrably effective for a subset of procedures.
So here we see another CDC[?] core strategy. This one is aimed at surgical site infection prevention practices. Here they call out select high-risk procedures using the examples of cardiothoracic, orthopedic and neurosurgery for decolonization, and again specify CHG bathing plus mupirocin or povidone-iodine. But the bottom section, that supplemental strategy and asterisked[?] statements are actually kind of even more interesting. Facilities can choose to apply the selected pre-op course or source control regimen universally to all patients, or they can screen patients undergoing high-risk surgery with a test that detects both MRSA and MSSA, and then provide the decolonization regimen only to those who are staph aureus positive - and we're going to get back to that.
So as I mentioned, this is not all about acute care and that's not the target audience here. We know that the dynamic of healthcare delivery is shifting - it's actually shifting even more rapidly than we predicted three short years ago. In 2020, we saw 5,930 Medicare-certified ambulatory surgery centers perform upwards of 5.6 million procedures in over 18,000 procedure areas. There's absolutely no reason to believe that this growth will diminish or even shrink anytime soon. But along with that, the recent MedPAC report to Congress discussed the need for[?] early efforts to develop a value-based purchasing program for this setting. In the same report, they say, quote, "In general, a surgical site infection measure could be used to track infection rates for ASCs and identify quality improvement opportunities for ambulatory surgeries conducted in HOPDs and ASCs. In addition, measuring SSI rates could encourage providers to collaborate and better coordinate care for ambulatory surgery patients." End quote.
When I read this, my first thought was, "Wow, that should be fun." But aside from this, a forthcoming pay-for-performance model in the ambulatory setting, your reputation is really your currency, much like an infection preventionist's currency as their credibility. Credibility and reputation are hard to earn and easy to spend or lose, and adverse patient outcomes will undermine and cost a facility patient volume and revenue rather quickly. The best care yields the best outcomes, and the best outcomes yield higher volume. And so it goes.
Speaking of volume, this graph was issued in early 2020, but the Becker's ASC Year in Review of 2020, which was actually issued in - I think it was October 2021 - seems to suggest that the rate of growth may have been underestimated. While many aspects of health care delivery were contracting during the pandemic, ortho cases grew 21% and total joint reductions doubled from the year before.
In the first five months of this year, 2022, the AORN Outpatient Surgery periodical has had two articles that addressed the need for, and the benefits of, a nasal decolonization program specific to the ambulatory surgery setting. In both, the authors extrapolate what is known from the acute care setting and encourage ASCs to perform a risk assessment as well as evaluate the need for, and benefits of, an active decolonization program.
In a high-volume setting, as we find with ASCs, it makes sense to use a nasal decolonization regimen that can be, frankly, clinician-applied - once, preferably - and therefore verified before the patient actually undergoes the procedure. A recent article by Safdar and colleagues on my own home turf of UW here in Mass, recently looked at the human factors element of deploying nasal decolonization in not only acute care but in ambulatory surgery center as well. It found that the barriers to implementation included some probably really familiar themes to you all, including a lack of effective communication, insufficient information and lack of systemic implementation. Once they course corrected, they found that the program was implemented smoothly and without adverse effects to patients.
So let's get into the "how" a little bit, shall we? While there is largely uniform agreement on the method of skin decolonization, namely CHG bathing, there are two broad categories of nares decolonization: antimicrobials and antiseptics. With antimicrobials, the most well-studied example is going to be mupirocin. It has, as I mentioned previously, a limited spectrum. It's a cream or an ointment that's usually applied multiple times over the course of several days. And, as with all antimicrobials, resistance can, does develop and can increase. With antiseptics, we have a couple of examples, including povidone-iodine as well as alcohol. This is an interesting technology that's not available in the US currently with photo disinfection, but the difference is that antiseptics have a broad spectrum. They're effective against bacteria, fungi, protozoa, viruses - it's great. It's usually in a liquid formulation. It's usually applied once immediately prior to the procedure. And in contrast, there has been no resistance reported.
So we dive into the traditional model, specifically for staph aureus. It has looked at decolonization of the interior nares with mupirocin ointment, which is also known as Bactroban. Mupirocin is a carboxylic acid class of antimicrobials. It was actually discovered in 1971 after they derived it from pseudomonas fluorescens. It was then developed and released in the market in 1985, and the first times we heard about mupirocin resistance was two years later, in 1987. As of 2018, the wholesale cost of a 15-gram tube is $2.50 and it retails for $25. And the standard decolonization protocol for using this ointment is for patients to self-apply to the interior nares twice daily for five days, all prior to surgery. And it's important to note there is limited - actually, virtually no data - demonstrating the effectiveness of a single application on the day of surgery.
Despite its really good evidence, it's not a panacea. This study from 2020 may have gotten overlooked, because people were kind of busy in 2020, but it offers an interesting insight into the issues of patient decolonization at home for five days prior to their scheduled surgery. In this study, researchers actually enrolled 421 scheduled cardiac surgery patients. They screened them for staph aureus, they prescribed the decolonization regimen of CHG bathing, antiseptic mouthwash as well, as well as the five days of mupirocin therapy for known carriers. Notice in this population there was an ideal condition of zero mupirocin resistance. They had none. But despite this - despite this, everything being perfect - the therapy actually failed 26.2% of the time. Incidentally, they also missed a third of their other patients because the cases were emergent for cardiac surgery - no surprise there. And lastly, of the patients who tried and failed decolonization, 10% of them developed immediate sinusitis[?].
But it's not just effectiveness we have to worry about. We also have to worry about resistance, which actually contributes to effectiveness. So it was introduced in 1985. Resistance was reported in 1987. But how resistant is it in the population that it's targeted for? Well, the honest answer is it varies widely. In a more recent population analysis across multiple California facilities, the prevalence of resistance of MRSA [inaudible] mupirocin was reported as high as 12.6% by Wong[?] and colleagues back in 2019. Interestingly, and not surprisingly, the level of resistance seems to increase the more that mupirocin is used. In a healthcare facility in Montreal, over the course of four years, the level of resistance increased from 2.7% when they started to 65% four years later, following their use of a universal decolonization program. Stateside in 2007, a large healthcare organization in Illinois began a similar decolonization program for controlling MRSA, and they found that nearly a quarter of their isolates were resistant.
So while the evidence is strong in support of decolonization regimens using mupirocin, there are issues. The first is the timing - the need for five days of therapy before effectiveness, and how surgeries don't always give patients and providers that much notice. The second is that self-application by patients requires that they have sufficient ADLs, or activities of daily living - in other words, that they can self-apply. And then the third is that, as with all antimicrobials, they are targeted towards specific organisms - like I said in this case, staph species - and that SSIs are caused by more than just these targeted organisms, and that over time, resistance develops. Isolates that are resistant? Well, the antimicrobials don't work on them. But even if they are susceptible, it may not work up to 26.2% of the time.
So if antibiotics may not be the best choice for failure rates baseline because of failure rates and baseline and increasing resistance, maybe we should look at the antiseptics as an option. Let's start with the alcohols. It covers many vegetative bacteria, viruses and fungi, and while its action is immediate, its degree of persistence is questionable. In other words, it kills these organisms immediately, but the surface - or in this case, the nares or the nose - can be quickly and easily recolonized. I like to think it's analogous to alcohol-based hand rubs or hand hygiene agents.
So this is a single center small study. In this, the researchers focused on MRSA colonized patients. In the first comparison, colonized patients were administered either a commercially available alcohol-based antiseptic to the nose in a single dose, or a phosphate-buffered saline as a placebo. There was no statistically significant difference in organism recovery between these two groups. When they actually repeated this and applied the alcohol antiseptic three times over a three-minute period, MRSA was recovered less commonly in the treated group to a statistically significant degree at ten minutes, and then again at two hours, but actually lost statistical significance after two hours. And this finding reinforces what we know about alcohol: that it's broad spectrum - despite only having measured MRSA in this group - it's fast or rapid, but it's really not persistent.
Well, in 2014, researchers from the Medical University of South Carolina recruited, screened and enrolled 39 healthcare workers that they knew were colonized with staph aureus. They applied an alcohol-based solution or placebo to the nose at the start of the employee shift. They had them reapply it four hours later, reapplied it again four hours later, before they tested the employees ten hours into their shift. So three applications, all before ten hours.
In this limited study following three separate applications during a single shift of work among what I would describe as presumably healthy adult health care workers, they saw an overall reduction in staph aureus colonies of 91%. Now, notice they actually used a chromogenic agar for testing, with reported sensitivity of only 86.6%. But this doesn't actually look at patient outcomes.
In 2017, researchers at Baylor Orthopedic and Spine Hospital in Arlington, Texas, reported a pre-post analysis of spine surgery infections exclusively to staphylococcus species organisms. In the pre-intervention phase, they decolonized all spinal surgery cases with CHG bathing and mupirocin. That mupirocin was applied at home with the five days, obviously, pre-operatively. And during the intervention they continued the CHG bathing but they stop the use of mupirocin, while the staff applied the alcohol-based nasal treatment pre-operatively three times daily during any admission, and instructed the patient to self-apply three times daily post-discharge for up to seven days. Staff were also encouraged to self-apply, in other words, to decolonize themselves in the same nares decolonization regimen, and their self-reported compliance with this was actually pretty high. That's pretty good. The net result was an 81% reduction in SSI rates due to staphylococcus.
However, this study had a few concerns. First, the CHG bathing got better during the intervention, although it was just 8%. But secondly, that baseline period of October 2014 through June 2015. Well, in 2015, the national rate of infection for all adult laminectomy and spinal fusion cases nationally was 0.55 per 100 procedures. In other words, about one SSI per 200 procedures. The baseline for staph infections only in this study was three times higher, with 1.76 cases per 100 procedures. In other words, about three-and-a-half infections per 200 procedures. These opportunities for confounders and what's called regression to the mean really can't be overlooked. If you have a really high rate when you start out, there's a really good chance that you're going to be able to get that rate down regardless of what you do.
Well, then there's this last one, though. And that's really the $64,000 question. In [inaudible] in 2020, researchers at UHS in Pennsylvania took a first stab at this, where they decolonized patients with an antiseptic, but they stopped isolation precautions. But their outcome of measure of success, aside from the obvious financial and staff satisfaction, was kind of a blunt tool. They used MRSA lab ID event, which, while a proxy for MRSA infection and transmission - by the way, MRSA lab ID event just means positive blood cultures due to MRSA after you've been in the hospital for a couple of days. So it's supposed to be a proxy for MRSA infection and transmission, but it's really a far cry from answering the question if this is a safe and effective practice.
The right way to do this - actually, the right way to look at this would be to do a true quasi experimental study where a facility performs admission, discharge or transfer cultures - you know, in case any of you out there have some free time and want to work with an acute care facility. Your baseline would actually have true MRSA acquisition data. Your intervention would be to use a nasal decolonization agent and routine patient regimen with something like a CHG, plus or minus an antiseptic oral rinse, as well as a suspension of contact precautions. You would compare your MRSA acquisition data pre and post, and then importantly for control variable, you would pick something like another MDR, like VRE, for example.
Why would you need VRE? Well, first, a true quasi experimental study actually requires it. But more importantly, this would actually help answer the relative contribution of your multi-focused intervention, right? I mean, if MRSA and VRE both go down and they decrease by about the same amount, well, it's hard to tease out the role nares decolonization or nasal colonization did over and above the CHG bathing regimen - which, arguably, might well impact VRE. But if either VRE stays the same, or it goes down but goes down by a lesser amount, then you might make the argument that nares decolonization is actually not - is actually critical. And of course, if they don't change, then it obviously doesn't work. But that's really the right way to answer this question. I hope somebody is actually working on it. If it does work, it would not only be cost effective, but at nearly $160 a day, it would probably be cost beneficial. And to be honest, your staff would really actually love you, because nobody likes putting on gowns and gloves every time they go into a patient room.
Well, let's switch gears. Interestingly, iodine was discovered in 1811 by a French chemist. His name is Bernard Courtois, who is actually also partially credited with synthesizing morphine from opium. So there you have it, antisepsis and pain management for the incision and recovery all in one. This led to the synthesis of povidone-iodine by industrial toxicology labs of Philadelphia in 1955. It's bactericidal, biocidal, fungicidal, with no demonstrable in-vivo resistance. Persistence estimates vary, but most evidence suggests that it's less than the chlorhexidine gluconate and alcohol like CHG, which is not commonly recommended for the nose anyway, but it can be persistent for as long as 12 hours. In terms of allergy, this comes up a lot. In fact, the best study that's been done that looked at this looked at a study of 500 healthy adult volunteers and showed an allergic response to a patch test of 10% povidone-iodine in only two patients, or a rate of 0.4%.
On this study of over 1,500 patients undergoing primary revision arthroplasty, the researchers randomized patients to narrow colonization within either five days of mupirocin or a single application of a 5% povidone-iodine, with both groups undergoing CHG bathing the night before and the morning of. Although SSIs due to any pathogen were half as common in patients decolonized with the iodine, this finding was not statistically significant - a P-value of 0.06. Now, that's kind of funny because we put a lot of emphasis on P-values and the difference between a P-value of 0.06 versus a P-value of 0.04, actually, in pragmatic approach, doesn't actually - it's not a big difference, but technically it's referred to as statistically significant.
Staph aureus deep SSIs occurred in five of the 763 patients undergoing mupirocin decolonization, but none of the 776 patients receiving the povidone-iodine. Interestingly, the same authors noted in the prior publication, unrelated to this study, that they historically decolonized patients with mupirocin, and in a survey of 146 patients found that - 93% of respondents found the CHG bathing protocol easy or very easy to comply with, but 54% said the out-of-pocket expense for the mupirocin prescription was burdensome, and 19% of them actually decided not to do it. Unrelated to this study, as I mentioned.
Well, this study of over 700 veterans who underwent elective orthopedic procedures was it before or after retrospective nonrandomized trial with matched historical controls. Their decolonization protocol involved both CHG bathing as well as a CHG oral rinse the night before and the morning of surgery, and a 5% povidone-iodine nasal application on the morning of surgery. Their historical baseline had a surgical site infection rate of 3.8 per 100 procedures, which dropped rather dramatically to 1.1 per 100 procedures, following initiation of the decolonization program. In a multivariate logistic regression analysis, decolonization of patients was found to have a protective effect in avoiding any SSI within 30 days of surgery, with an odds ratio of 0.24. But of course, this study is limited to a single facility as well as being among veterans.
And this is just another more recent report from the field. This time this is at Duke Raleigh Hospital in North Carolina, and while the study's design in and of itself is lacking because it's a before or after study without a good control arm, they showed a 60% decrease in SSIs of elective orthopedic, hip, knee and spinal fusion cases, and a greater than threefold lower overall rate of SSIs compared to their non-orthopedic procedures.
I like to bring this up, because it shows that nasal decolonization doesn't just benefit in acute care or the ambulatory surgery care. The protect study was actually headed by Dr. Susan Wong at the University of California Irvine. They enrolled 24 nursing homes. Nursing home residents were administered either - were administered povidone-iodine to the nose twice daily for five days every other week. And they took out all the bathing products and replaced them with CHG. Interesting, the compliance with this protocol was really not perfect. It ranged across the three facilities and two treatments between 61% and 93%. There were 11 intervention facilities with 13 controls. And on average, 49% of the 1,400 residents cultured at baseline were recolonize with any MDRO, and half of those had more than one multi-drug resistant organism. And this intervention lasted for a year and a half. All the MDROs decreased in the decolonization treatment group by about 36%, and in multiple logistic regression, decolonization was a protective factor against any drug-resistant bacteria individually for each organism, with the exception of CRE, or carbapenem-resistant enterobacteriaceae. The authors actually concluded that this universal decolonization protocol, if it was deployed regionally, had the potential to decrease drug-resistant organism acquisition, infection, antibiotic use, and ultimately overall regional drug-resistant organisms spread to other healthcare facilities throughout the region.
Povidone-iodine is available in a wide variety of formulations, specifically as it relates to percent concentration. A common povidone-iodine oral rinse that's actually used in Europe has a 0.5% formulation, while swabs available in the US are most commonly either 5% or 10%. As part of this study, researchers took a single nursing home, they replaced the 5% formulation that was applied with two swabs per nose twice daily, with a 10% formulated single swab per nare, applied twice daily, and they monitored nasal decolonization and found that they had identical percent reduction in carriage between the two regimens.
Well, does it work? Well, for every study, there's always going to be another study that comes along and says, maybe that's not right. But in the small, single-center study, MRSA colonized patients were randomized to 10%. povidone-iodine or a placebo. In neither group did they use CHG bathing as part of the decolonization regimen. And they found that the iodine group netted a significant log reduction in MRSA recovered at one in six hours after being applied, but that significance did not continue beyond the six hours. In a subset of this population, they took 18 individuals and randomized them to a placebo or continue the iodine application every 12 hours for upwards of five days. And while there were fewer MRSA colonies recovered from the treatment group two days after that last dose, this finding was not statistically significant, nor was carriage eradicated.
But I would say the important part of this study is that 90% of all the patients in this study were colonized with MRSA in anatomical sites besides the knowns. But as I mentioned, they had no bathing regimen, including this protocol, and there was no description of the participants provided. Translocation of organisms from one anatomical site to another is likely through self-inoculation. That's why decolonization protocols almost always include CHG bathing.
Now, the overwhelming evidence suggests that colonization does predispose patients to infection during their hospitalization, and often as a result of the medically necessary interventions that I mentioned earlier, if you bypass the body's actual defenses through incision, intubation or intravascular cath access, you're going to introduce some of those colonizing organisms to a new and rich environment which causes infection. Of course, we know that HAIs increase the risk of significant morbidity and mortality - again, most of this is reported in hospitalized patients. But what about persons colonized in the community? I think this really applies to the ambulatory care setting. What about persons colonized in the community? In other words, what happens to them after they go home infection free? Does colonization matter then?
Well in this study, researchers looked at a weighted population estimate of over 118 million US adults between 40 and 85 years of age, a selection of which were colonized with staph aureus and MRSA way back in 2001 to 2004, and then they followed them forward in time for 11 years. And while it might not surprise you that patients that were colonized with MRSA were more likely to die, there was no association with staph aureus colonization overall.
This table from NHS then explains the cutoff for all relative procedures. In other words, if you enter a procedure duration greater than the allowed amount, the NHSN, which is the seller of HAI data collection group at CDC, actually rejects that entry, because it seems to most likely be a computer-entered error. As an example, if the interquartile range for an appendectomy is 42 to 100 minutes - so taking out your appendix is going to take between 42 and 100 minutes - the IQR 5 is the value of the 75th percentile plus five times the 25th percentile of 42 minutes. So you take the 100 minutes plus the five times 42 minutes for a total of 210 minutes, or 3 hours and 30 minutes. In other words, the CDC says that no appendectomy case should take that long.
So in looking at this list, you can see that these monstrously-long procedure times are two to three-fold higher than most any realistic scenario. If decolonization is a treatment to reduce organism density during high-risk time periods, then persistent suppression of organisms needs to meet that threshold, but it doesn't necessarily need to go beyond that threshold.
Well, let's shift gears again. What about the patient? What do they want? Well, arguably they want safe medical care, free from infection. I'm not going to provide you with a literature reference here because it's pure common sense. No one goes to the provider hoping for an unanticipated healthcare-associated infection. So how do they best wish to avoid it? Well, in a 2014 study of over 1,600 patients, patients preferred clinician-applied nasal decolonization protocols over and above that self-administered five-day decolonization regimen of mupirocin. But what else matters? Does patient comfort or provider preference matter? I mean, arguably smaller, equally-effective applicators can make a difference.
Infection prevention is not 5% knowing what to do and 95% figuring out how to get it done. It really comes down to human factors, and the more complex the system is, the more difficult it is to effectively implement. So let's look at one of the most common pre-surgical decolonization protocols we use today - what I'm going to call the "test-and-treat" program, where you screen or test patients before the procedure, decolonizing with a common strategy like mupirocin CHG bathing for five days prior to their elective procedure. First, if a program is only screening and decolonizing patients undergoing select procedures like total joints and cardiac, a decision point has to be reached. Does the patient meet criteria for the screening into[?] your program? Are total joints inclusive of revisions? Is a cardiac cath procedure really a cardiac procedure? I mean, you can use decision support systems to help, but it's still a decision point.
Next, you have to place an order for the screening. Sometimes this is done by a nurse during protocol or requiring a provider co-signature. Sometimes it's the provider themselves that enter the order. And here too order sets[?] and decision support can help, but it's still an opportunity for error. Anyone who's received a call from the lab knows that specimen collection and transport is not a joking matter. It has to be collected properly, labelled properly and transported appropriately. We're going to talk about the lab in a second, so we'll skip over that for a second. But once a result is actually made available, someone - and often the provider - needs to review the result. If it's positive, the treatment needs to be ordered by the provider. Of course, there can be standing orders here too. And nonetheless, someone needs to notify the patient, provide direction and instructions, and then the patient needs to go to a retail pharmacy, they need to pick up and purchase, sometimes out of pocket, that decolonization regimen. And with the aforementioned decolonization protocol, the patient has to self-administer the treatment to themselves over the next five days. And this again assumes a degree of autonomy and sufficient activities for daily living in order to accomplish this. And lastly, the treatment has to be effective - in other words, there can't be any resistance, as I talked about earlier. Of course, all of this works if and only if the procedure is elective, planned five days out - which we know doesn't always happen - and even when all these systems are in place, you still stand a 26.5% risk of failure in terms of effectiveness.
While we assume the lab test results are the end all, be all source of truth, the fact is that they are all susceptible to testing, sensitivity and specificity, and to be honest, the cost of the test itself - and certainly no lab test is perfect. The gold standard for laboratory testing for nares screening is culture-based method, which can take up to 72 hours, and of course in the[?] lab-based method, less than 100% sensitivity can mean that some patients colonized with organisms are actually missed.
I love math. If we take the inverse of the reported sensitivity measure, multiply by the proportion of expected staph aureus colonized patients, we can actually estimate the number of staph aureus patients who our detection method is going to miss. These numbers are based on universal decolonization of all surgery patients and organizations I would argue most of us would really highly recommend[?]. A selective chromogenic [inaudible] shown here has a reported sensitivity of 86.6%. With the volume of surgery performed by the Mayo Clinic, that means that every year, 2,110 patients with staph aureus in their nose undergoing surgery will not be decolonized if their decolonization strategy was for all surgical cases. Does a $21 lab test negate the cost of universal decolonization? And that $21 is just laboratory supplies alone. Well, it really depends on the volume, prevalence, but this is certainly a question worth asking.
Speaking of questions worth asking, universal strategies are not without their own challenges. For example, if an organization moves from targeted staph screening of patients to universal decolonization, there's going to be questions. Which antibiotic prophylaxis should I use if I'm not aware of their MRSA status? And this is how TriHealth in Ohio addressed this issue in the acute care setting when they suspended their screening program in favor of universal decolonization. And as you can see, they use traditional MRSA risk models to determine whether the surgical prophylaxis warranted potential MRSA coverage.
Well, further bringing it full circle, where do HAIs actually come from? Obviously they come from the environment. Patients harboring drug-resistant organisms discharged from rooms under good environmental clean protocols are still more likely to transmit their pathogens to the next admission. That's a topic for another presentation. Infections can come from healthcare worker hands, also related to the environment, not to mention the frequency with which healthcare workers themselves, under the weather, continue working and potentially infect others, as we've seen time and time again. That's also for another presentation.
But patients can infect themselves. Their microbial flora serves as a source, the procedures we perform the conduit, and undoubtedly their flora serves as the vector for the next admission to the same space, and tangentially[?], via healthcare worker hands. In the map of determining your source of infection, what role does the individual patient play through no fault of their own? What are you doing to make sure that their silent carrier status does not reach a pathogen destination?
So let's consider our conversation today. Humans carry organisms, and organisms can cause disease. Obviously, reducing colonized organisms can reduce the risk of infection, and patients want to be safe and use something that actually works. And while antimicrobials target specific pathogens, resistance can undermine this. Whereas antiseptics target multiple pathogens and have no resistance, the choice of who to target can be undermined by human factors and testing limitations. So the summary includes many of the same points that I just covered, as well as the fact that the ambulatory care setting, especially the ambulatory surgery centers, have seen a dramatic increase in volumes, especially orthopedic procedures, with ongoing projected near-exponential growth in coming years. Interestingly, the American Association of Orthopedic Surgeons does recommend nares decolonization, and hopefully if you're doing orthopedic procedures, you're already on board with that.
So I would once again like to extend my heartfelt gratitude and thanks to McKesson for the opportunity to share this information with you today. My contact information is here, should you have any follow up questions or concerns. And obviously, if time allows, I'd be happy to take your questions at this time. Thank you.
Brandon Martin: Thank you so much, Marc-Oliver. We do have one question that that came in. I believe we've got time just for one. So, yeah, this person asks, "Could nasal decolonization protect us from COVID-19?"
Marc-Oliver Wright: What a great question. So I'm going to say a couple of things here real quick. So one, there is one paper that looked in vitro - in other words, in a laboratory setting - as to - actually there have been more than one paper that I have looked at the in vitro effectiveness of antiseptics like povidone-iodine, and specifically povidone-iodine in killing coronavirus. And those studies have consistently and mutually showed a benefit for nasal decolonization in terms of the in vitro setting.
I would also point out that some researchers have proposed protocols in the operating room. So Loftus from the University of Iowa had a great paper back in 2020 where they effectively describe their efforts to limit the potential for transmission of COVID-19 in the operating room. And they endorsed the use of something along the lines of nasal decolonization, specifically the antiseptics. Now, if you're using mupirocin, again, mupirocin is effective against staph. It has no virucidal activity, so it's probably not going to be effective. But the antiseptics, and specifically the one that's probably been the most studied, being povidone-iodine, has shown some benefit.
Now, do you have any recommendations or instructions for use for manufacturers that talk about their nasal antiseptic agents and using them for COVID-19? Not that I am aware of, but I would suggest looking or even as simple as Googling nasal decolonization or povidone-iodine and COVID-19 prevention. Great question. Love it.
Brandon Martin: Yeah, that's really fascinating. Well, again, we are out of time, and I just want to thank you all for joining us today. If you do have any additional questions, please feel free to reach out. I'd also like to invite you to visit our website at mms.mckesson.com/educational-webinars, and that is where you can opt in, see additional webinars that are coming up. And I do encourage you to take a moment to opt in so that you'll receive invitations and announcements for future webinars.
Marc-Oliver, thank you so much for joining us today. I really appreciate you sharing your time and expertise with us. And to all of you attending, thank you so much. Check your inboxes in the coming days for a replay of this event as well as a PDF file of Marc-Oliver's slides and some information about your continuing education credit. Our next webinar will be Remote Patient Monitoring on 15th June 2022, and you can register for that on the link that I mentioned earlier. Again, Marc-Oliver, thank you so much. I really do appreciate your time.
Marc-Oliver Wright: Thank you. It was a pleasure.
Brandon Martin: Have a great day, everyone.
Webinar originally aired on May 25, 2022
© 2022 McKesson Medical-Surgical Inc.