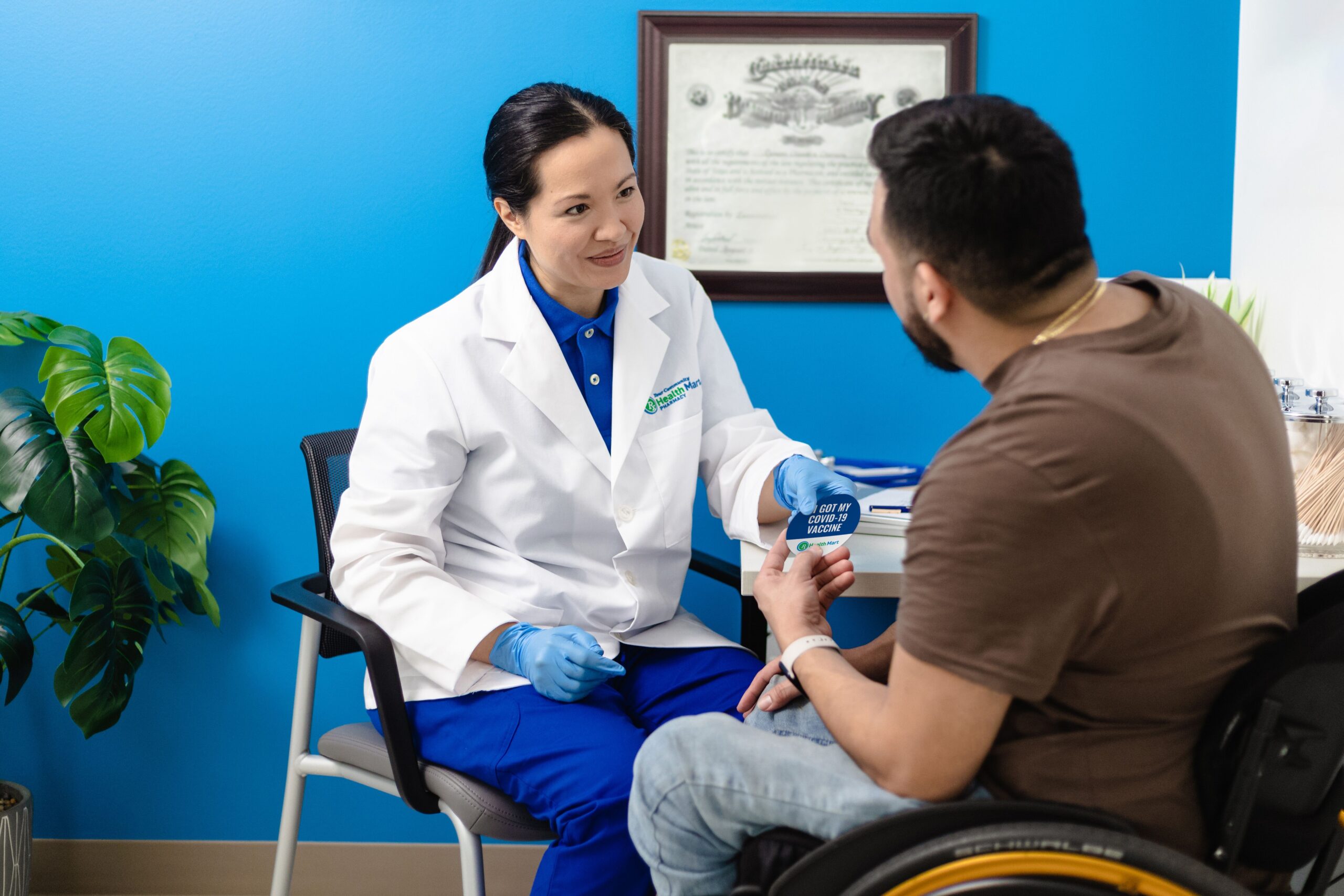
- Respiratory Care
Deliver the right care for respiratory conditions
Offer and administer vaccinations, diagnose quickly and confidently with point-of-care lab tests and provide treatment with branded, generic and over-the-counter medications

Help Your Respiratory Patients Breathe Easier
Respiratory season begins each fall but you can count on us to keep you prepared all year round. We understand the importance of providing quality respiratory care to your patients, and we have a wide range of resources and products to support you throughout the season, and beyond.
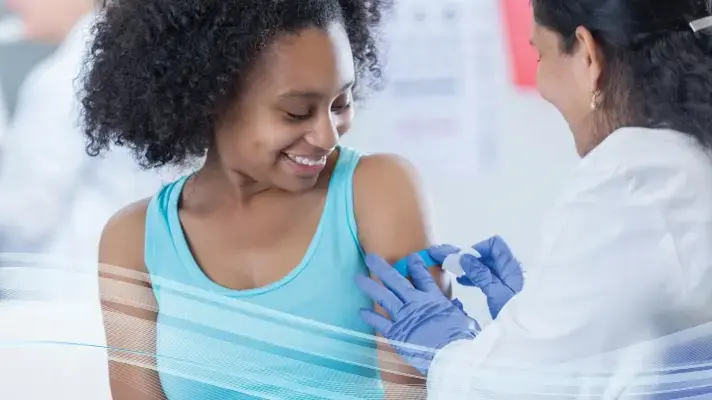
Prevent
McKesson Medical-Surgical has an extensive portfolio of vaccines available for respiratory illness prevention, including flu and traditional core vaccines. We also have new vaccines available, including COVID-19, RSV and Prevnar 20 vaccines. And as your single source for your respiratory needs, you can find the products you need across the spectrum of infection prevention, like masks, hand sanitizers, wipes, PPE, Band-Aids, alcohol prep pads, and needles and syringes.

Diagnose
Be prepared to diagnose common respiratory conditions this season with point-of-care lab equipment and tests. We offer a wide variety of products like our lab analyzers, additional assays/tests and test kits. No matter the size, scale or complexity, McKesson Lab helps you gain access to quality lab results so you can provide efficient care to your patients with quick diagnoses.

Treat
Stand up to respiratory illnesses this season with McKesson’s extensive selection of asthma treatments, anti-viral medications and over-the-counter medications. We also offer respiratory equipment from leading respiratory manufacturers across key device needs, including ventilators, oxygen, nebulizers and CPAP. Experience the convenience and peace of mind that comes with sourcing your respiratory needs from a single distributor.
Prevention Resources
Strategies for combating vaccine hesitancy
Explore different tactics for addressing vaccine hesitancy, such as educating yourself on new information and engaging with your patients regularly.
Your RSV questions answered
Stay up to date on the latest information on RSV, including how to test for RSV and updates on new vaccines.
Infection Prevention Program
Find out more about our infection prevention and control program, UPrevent™, your single source for building your infection prevention program.
Featured Prevention Products
Vaccinations
Infection Prevention

A robust respiratory program
- Help prevent respiratory illnesses by establishing a vaccination program for children, adults and seniors
- Teach your staff and patients effective infection prevention techniques to prevent the spread of disease.
- Check out these flu and respiratory resources to learn more about best practices, the latest guidelines and more.
Diagnostic Resources

Point-of-care lab testing
Point-of-care (POC) lab testing provides the information you need for quick, accurate diagnosis. When you test patients at the point of care, you can:
- Send patients home with same-day results and treatment plan
- Prescribe accurate treatment for multiple conditions and avoid unnecessary antibiotics
- Help reduce hospitalizations with correct diagnoses the first time
- Distinguish an active respiratory infection from past exposure to COVID-19
Choose the right testing for your respiratory patients

Molecular Testing
- Tests include influenza A & B, strep A, RSV and SARS-CoV-2
- Detects an active infection
- Instrument-based test
Benefits of molecular testing:
- Let patients know if they are infected, so they can be prepared and prevent transmission
- Understand how best to treat the patient’s illness and reduce transmission
- Feel confident in your diagnosis with highly accurate test results
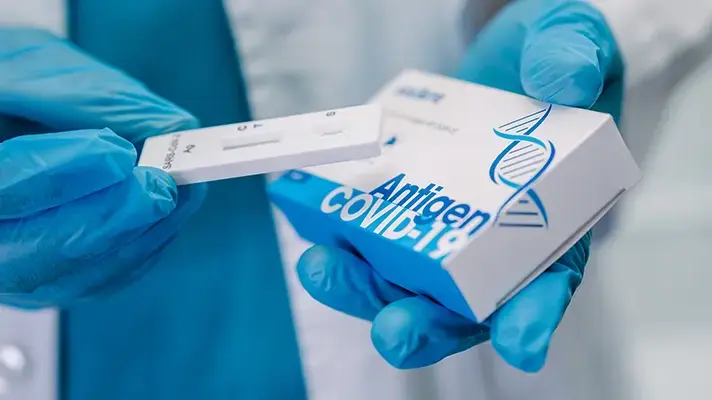
Antigen Testing
- Tests include influenza A & B, strep A, RSV and SARS-CoV-2
- Detects an active infection
- Reader, instrument or rapid cassette-based test
Benefits of this type of testing:
- Plays an important role for the early diagnosis of SARS-CoV-2, particularly in situations with limited access to molecular methods.7
- Let patients know if they are infected, so they can be prepared and prevent transmission
- Understand how best to treat the patient’s illness and reduce transmission
Featured Treatment Products
Stand up to respiratory illnesses this season with McKesson’s extensive selection of asthma treatments, anti-viral medications and over-the-counter medications. We also offer respiratory equipment from leading respiratory manufacturers across key device needs, including ventilators, oxygen, nebulizers and CPAP. Experience the convenience and peace of mind that comes with sourcing your respiratory needs from a single distributor.
Pharmaceutical Treatments
Respiratory Therapies
Featured Respiratory Webinars
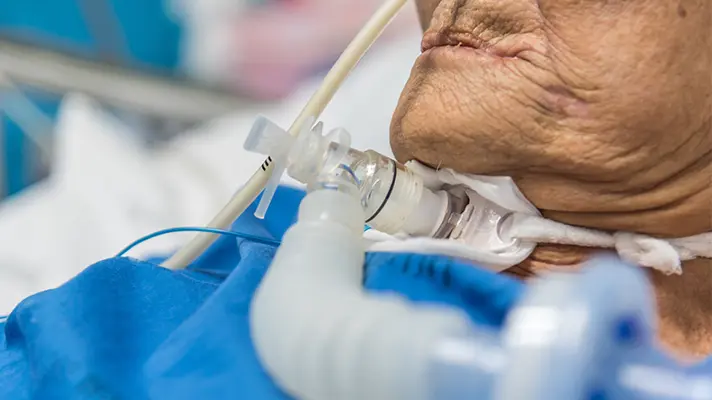
Handling your tracheostomy patients: An overview of tracheostomy care and consumables
Watch this webinar for an overview of tracheostomy care and consumables, including education and resources for those customers affected by the Shiley™ Legacy obsolescence.
Aggressive diagnostics can help you achieve:
Watch this webinar to review the advantages and limitations of current PCR testing options as compared to diagnostic alternatives, and learn how PCR testing can help improve patient care.

Contact us to learn more about our respiratory care solutions
1. https://mms.mckesson.com/content/infection-prevention/universal-standard-precautions/
2. https://mms.mckesson.com/content/reducing-hospital-readmissions/pneumonia/
3. https://mms.mckesson.com/content/respiratory-care/
4. https://mms.mckesson.com/content/wp-content/uploads/2024/02/the-roadmap-to-respiratory-season-success-in-non-acute-settings.pdf
5. https://mms.mckesson.com/catalog/category?node=403253
6. https://mms.mckesson.com/content/insights/how-point-of-care-poc-labs-help-in-preventing-the-spread-of-infectious-diseases/
7. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7263236/
Be advised that information contained herein is intended to serve as a useful reference for informational purposes only and is not complete clinical information. This information is intended for use only by competent healthcare professionals exercising judgment in providing care. McKesson cannot be held responsible for the continued currency of or for any errors or omissions in the information.
The product information contained in this document, including the product images and additional product materials, was collected from various supplier sources. All product claims and specifications are those of the product suppliers and have not been independently verified by McKesson Medical-Surgical or its affiliates (“McKesson”). McKesson is not responsible for errors or omissions in the product information. The properties of a product may change or be inaccurate following the posting or printing of the product information in the document, either in the print or online version. Caution should be exercised when using or purchasing any products from McKesson’s online or print documents by closely examining the product packaging and the labeling prior to use. Due to product changes, information listed in this document is subject to change without notice. This information is placed solely for your convenience in ordering and McKesson disclaims all responsibility for its completeness and accuracy, whether or not the inaccuracy or incompleteness is due to fault or error by McKesson.
©2024 McKesson Medical-Surgical Inc. All trademarks and registered trademarks are the property of their respective owners.